Rhinoplasty Post-Operative Information
Overview
The below outlines what to expect following a rhinoplasty with me. You will be told if there is any variation to this, but by far, most surgeries follow this course. Most of my patients see me weekly for the first four weeks, then a month later, three months later and finally 6-7 months later. All post-op visits are not charged, regardless of how frequent they need to be. The goal is to achieve the best result possible, and some cases require closer, more frequent follow-up than others.
Initial post-surgery experience
When you wake from your surgery in the operating theatre recovery room, you will have a rigid external plastic cast taped over your nose (glued to small adhesive strips) and a small gauze taped under your nose. You will have a cold eye mask applied as you wake, and the nurse will check your comfort and get you to rest with your mask on. You will have small silicone stents (Splints) inside your nose that keeps everything locked in position over the ensuing days as you get slightly swollen. These splints do allow you to breathe on waking up and continue to breathe for 2-3 days following your surgery, although after that, they usually block up, and you have to wait for them to be removed at your first post-op visit to breathe well again. The splints just have one suture (stitch) holding them in just a little inside the nose.
Daycase or overnight stay
Most of my rhinoplasty patients go home the same day as their surgery (Daycase) but in some instances an overnight stay is planned and I will discuss this with you.
Transition to day surgery
Typically after 30 minutes or so in recovery, you will be transferred to the stepdown recovery/day surgery. Here a cool mask will continue to be applied, you can get up and go to the toilet if needed and have something light to eat.
Swelling management
These eye masks I supply you with are to go home with you and continue using as much as possible for three days postoperatively. The masks are like an ice pack but have the eyes cut out so you can read or watch TV as you rest up. Try to wear them non-stop for this period, only having them off to refreeze the mask.
When you first arrive home, I encourage you to apply a packet of frozen peas (or similar) over your eyes for an hour or two while you freeze your mask. Swelling increases for 3 days following surgery (any trauma or significant injury), and keeping things cooled definitely helps, especially at the very start. Go to sleep at night with your mask on and then get the bag of peas on again come morning, just for 3 days.
Less swelling speeds your recovery, reduces pressure and pain and reduces potential nasal framework distortion. Bruising can be reduced. This routine is the most important thing you can do for yourself in these first few days.
Nasal care
The gauze taped under your nose may need changing 3-4 times overnight mostly after some movement (e.g. going to the toilet). Most people only need the gauze in the first 24hrs to catch a little ooze. Please reapply it at home if needed rather than continually dab at your nose as your nasal skin is very delicate, your nose will be a bit numb, and tissues can be quite abrasive and damaging over time.
Contact me if significant ooze persists beyond 3 days. You DO NOT have any packing up your nose that needs removal.
Your nose will start to block over this time, which is annoying, but it will be fine after your splints are removed on your first visit. Be patient, and definitely DO NOT poke anything up your nose to try and unblock it.
Hospital discharge and medication management
- Pain Medication: To manage any discomfort following the surgery (see below).
- Bactroban (Mupirocin) Ointment: This ointment treats skin infections and promotes healing (see below).
- Antibiotics: These are crucial for preventing postoperative infections. Please ensure to complete the full course, which typically lasts for 10-15 days.
Bactroban (Mupirocin) ointment instructions
You will be provided with a tube of Bactroban (Mupirocin) ointment. Place some of this onto a cotton bud and apply it a small distance (5mm or so) up your nostrils over the front of the hard silicone splint, as per the picture below.
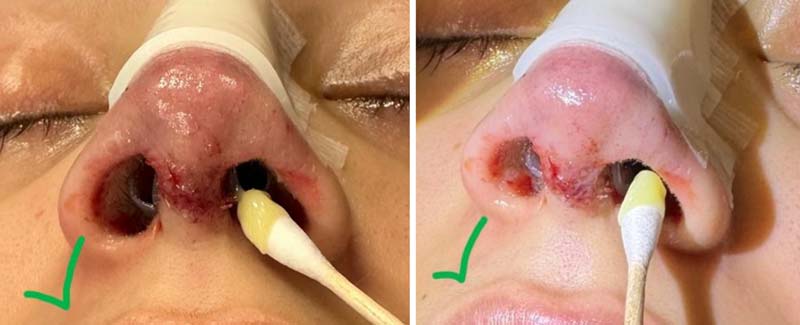
Do this twice a day, starting on the first day after surgery. This helps reduce crusting so I can easily access your splints to remove them when I see you. You will stay on this ointment for 2-3 weeks after your surgery until your nostrils no longer get crusty (once the incision line inside your nostrils has fully healed and stitches dissolved, the dryness and crusting stop). I will guide you in this.
The bridge of skin between your nostrils (Columella) has an incision that has been stitched and glued. This leaves a hard shell with a red/ purple tinge to it. Please DO NOT apply Bactroban (Mupirocin) ointment to this area. I want it to stay hard, supportive and protective. I will remove this glue at your second visit (10-12 days). DO NOT apply Bactroban (Mupirocin) to any external skin unless directly advised by me (as pictured below).
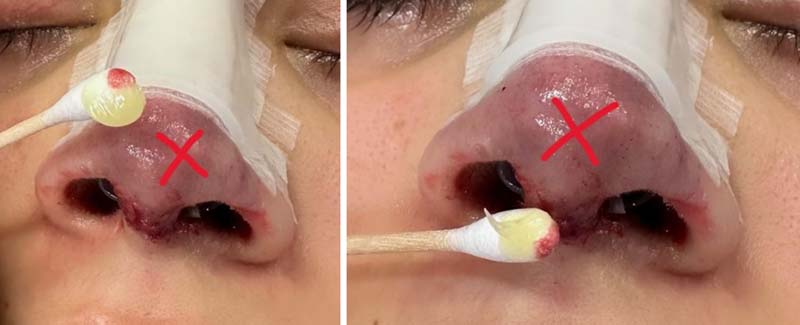
Nose cones

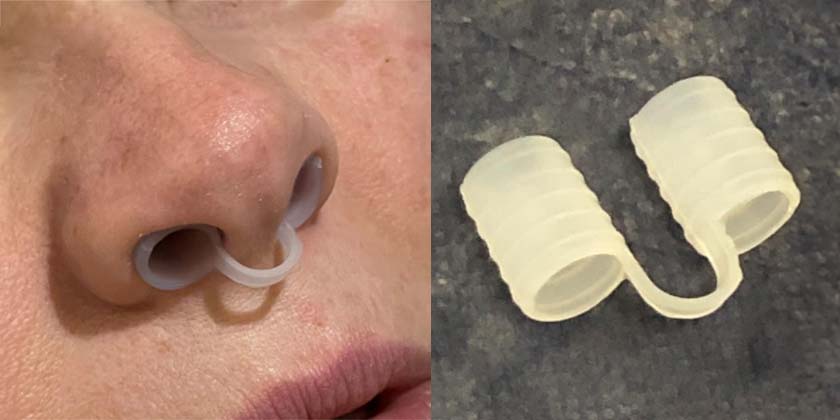
Silicone nose cones are small cylindrical stents that are placed into the nostrils, which I use during the rhinoplasty recovery process.
In this setting, their benefit is 3 fold:
- They help support the floppy nostril sidewall in the early stages of healing until it later tightens and stiffens to reduce long-term valving or sidewall collapse, which can be a major contributor to nasal obstruction.
- They help flatten the internal nasal incisions to maximise space.
- Lastly, and often most importantly to patients, they can help dramatically maintain and, in many cases, improve nostril symmetry.
They come in small and large sizes, and for a small nose, I may cut the side of a small cone and roll it up to make it even smaller. They come in smooth and grooved/ ridged. I prefer grooved, as they stay in better.
To insert them, I like patients to purchase forceps or tweezers (like eyebrow tweezers but without incurving—splinter tweezers or just bend eyebrow tweezers with pliers).
In front of a mirror, Squeeze the cone and insert it vertically with minimal resistance then release.
Don’t push them up open, or they can create a problematic shelf. If not fully up, reinsert. Generally, we want them flush with the nostrils. Once the first is in, do the second in the mirror. Get them sitting symmetrically, or they can create permanent asymmetries. Rotate each cone so the link does not place pressure on your columellar incision.
To remove the cones, pull on the link between them.
If you use kenacomb or Bactroban when using cones, the silastic will deteriorate quickly, and they will slip out more easily.
I usually start them at 2 weeks once your external cast is removed and like patients to use them as much as possible (20+hrs a day) for a week, then usually nighttime only for a variable time, often 4 weeks.
In complex cases, we may require them for months. The plan is adjusted case by case. A single pair will last two weeks before losing resiliency/ stiffness.
I like patients to remove them daily and wash them in clean water or even white vinegar every few days.
If you have any pressure/ pain/ bleeding, or concerns, stop using them and contact your surgeon.
You can contact our rooms for details if you wish to order more.
Pain management
Pain relief should be regular (4x a day) paracetamol, Celebrex (an anti-inflammatory that doesn’t affect your clotting unlike Ibuprofen) and some stronger pain relief such as endone (oxycodone) or palexia (Tapentadol).
Please take regular Celebrex for at least a week. Many people get by on just paracetamol and Celebrex but some may need some endone or palexia before bedtime for the first few nights while swollen. This is fine but if you’re in a lot of pain and require regular strong relief please contact me (see below).
Many of the rhinoplasties I perform are for those who have had surgery before (Revisions), have major trauma or just require a lot of reconstruction. Some of these cases require rib cartilage for reconstruction. This can be quite sore, and patients who have had this will be provided with a slow release stronger pain relief (Targin or Palexia SR).
I typically put on a course of oral cortisone (Prednisolone) post-op to help with healing, swelling, and pain and reduce infection risk. Prednisolone can give some people insomnia, so take it in the morning (it’s a single daily dose) to reduce this. Prednisolone can also exacerbate heartburn in some. Notify me if this is an issue.
More commonly now, donor rib cartilage is used if extra cartilage is needed. No extra medications are required in this setting.
Please contact me immediately if you have any concerns about your medications, reactions, or significant pain.
Constipation
Endone and palexia will sedate and constipate you (take a regular laxative when on them, even as a daily dose, such as Metamucil, psyllium husks or coloxyl) and many get some nausea. However, this is less common when on just a single daily dose.
If constipation/ abdominal discomfort is not settling, please see your local pharmacist for their guidance or, if not, your GP. Once your gut becomes uncomfortable, you need to have your bowels opening within 24-48 hours, or you will become very sore and need emergency care.
Sleeping
Your nasal framework will be soft and mouldable for the first 3-4 weeks following rhinoplasty. Be gentle.
I encourage you to sleep on your back with pillows under your arms to keep you there and a little head up (2 pillows). Neck support pillows like you wear on long-haul plane flights are good. You can turn your head side to side but not roll onto your side/cheek. Most people are not back sleepers, and it can take a week to get used to it, but sleeping on your side can push your cheek into your nose and distort it.
Absolutely no stomach sleeping. Many people find this hard, but it is important. Persist, and you’ll get used to it.
Eyewear
While you have your external plastic cast over your nose, I do not mind if you wear glasses until it is removed in the second week. For the following 2-4 weeks, do not wear glasses as they will leave impressions/ depressions on your nose that, in some cases, can become pigmented and take a very long time to fade. If possible, wear contact lenses. If you must wear corrective eyewear, tape the glasses up to your forehead to take the weight off your nose or place some tape under the glasses to distribute the weight (1/2 inch steristrip or micropore). Try and minimise the time you need to wear them as much as possible. Don’t wear sunglasses for 6 weeks post-op.
For the first week
Here’s what you should do during your first week post-op:
- Apply cold eye mask for 3 days solid
- Apply Bactroban (Mupirocin) ointment inside your nostrils 2x day
- Rest up. No activity apart from walking around the house. You don’t need to rest in bed. Sitting up better. Watch TV or read a book. No exercise for 3 weeks (anything that raises your heart rate). You can wander around the shops or walk the dog after 1 week.
- Take your antibiotics and pain relief.
- Keep well hydrated and refrain from very hot or spicy foods.
- Clean your face with a cool face cloth, avoiding your nose area. Don’t get your tapes or cast wet. No hair washing until your cast comes off (at 12 days) unless you really must. It can be done in a hairdresser’s basin (some patients book in the hairdressers in advance). Just have warm (not hot) showers keeping your face and hair dry. Do not have a bath, as it can increase bleeding risk and swelling.
- Stay off all supplements such as vitamins, oils (evening primrose, fish oil etc.) and herbal remedies. You can restart these after 2 weeks, but many affect clotting and healing in the short term. I do not mind if people take a pro-biotic (VIVOMIXX or LifeSpace are good brands) as it can help settle some people’s gut when on antibiotics.
- Sleep with your head raised higher than your chest to reduce bleeding and swelling.
- DO NOT blow your nose, sniff, snort or try to clear it. DO NOT use any nasal sprays, saline sprays or saline rinses/ douches. You can start blowing after 2 weeks.
Is it expected that you will examine the underneath (Base) view of your nose a lot in these first 2 weeks after surgery, as that is the only part of your nose anyone can see. Remember it will be swollen, have stitches and glue in the tissues and an external cast and internal splints distorting the tissues. It will never look exactly the way we want it long term in these first 2 weeks. Be patient. If you have any concerns, it looks very dark/dusky or infected; please contact me.
Weeks two to four
- Continue resting and limit your physical activities.
- Avoid sunburns, as they can cause swelling. Sun exposure should still be avoided as much as possible.
- Continue taking care of your nose as instructed.
- You may have a follow-up appointment to remove stitches, splints, and/or packing.
- You will have a follow-up visit to evaluate your healing.
- You can start more vigorous exercises and heavy lifting.
- Avoid contact sports.
At your second post-op visit (10-14 days), I will remove your cast and the hard glue from the incision between your nostrils. If you have had a rib or dermis graft, the dressing for this will also come off. Nearly all your stitches dissolve, but I often trim some up at this visit. Your nasal breathing should be quite good by now. Nearly always, I recommend and fit patients with NOSE CONES during their recovery. These are small silicone stents you place up to support the nose and aid breathing while healing. I often start them at the 2nd visit, and you wear them for 1-2 weeks all the time and then nightly for 2-3 months. I will discuss this with you as needed.
After two weeks, you can wash your nose gently with a gentle soap (like Dove) or cleanser—no scrubs or strips for blocked pores. The glue under your cast blocks your pores, and your skin will take a week or two to settle down after cast removal, so give it time to let the skin breathe and be gentle on it. No skin treatments, sunscreen, moisturiser, make-up (incl foundation) or significant sun exposure for the first month. Your whole skin envelope has been lifted and needs healing time. Less is more. Please don’t cake it in moisturiser or Bio-oil.
Your entire nose will feel a bit numb and “Altered” for 2-3 weeks, and then the numbness will settle to a small zone over and in front of your tip. In primary rhinoplasty, this almost invariably settles over 4-5 months, but in some instances of revision, some numbness can persist, although it is rarely bothersome. Similarly, your nose will become quite firm over the first month and stay that way for 4-6 months. This is a function of scar tissue/ healing and the internal stitches (that take about six months to dissolve – I never use permanent stitches).
After three months
- You can resume all normal activities.
- Always apply a strong sunblock to your nose when you are in the sun.
- While your nose is mostly healed, the final results may still take several more months.
By six months, the nose has achieved over 90% of its long-term appearance (this figure depends a lot on skin thickness and extent of surgery/revision etc.), but it is after six months that the nose starts to soften, become more flexible, the skin feels more supple, and the upper lip stiffness fully passes. It may not change much in appearance over this period, but it feels much more like YOUR nose again. After a structural rhinoplasty, the tip may have persistent stiffness (esp if rib cartilage is used), but this is desirable in most instances.
Please remember that healing after rhinoplasty is a slow and gradual process. Some swelling may be present for up to a year or more. The final results of your rhinoplasty may not be apparent until a year or more after the surgery. Also, keep in mind that everyone’s body is unique and individual healing may vary. If you have any concerns during your recovery process, don’t hesitate to contact us.
When to contact me
- If you notice any increasing redness, increasing pain, a bad smell in the nose or concerns of an infection developing.
- If there is persistent ooze beyond three days or significant bleeding.
- If you feel your cast is digging in.
- If you are getting very anxious or stressed. Some people find having a blocked nose or the worry or the surgery or their results very upsetting. This can be worse when on medication or getting less sleep (from me forcing you to sleep on your back). Contact me. It may be just some reassurance or, in some cases, some medication to help with sleep or anxiety.
I often tell patients I am their GP for the first two weeks following rhinoplasty. This is not literal but is meant to emphasize that I want to know if you have any concerns or health issues at that time to make sure they do not impact our result.
An excellent result is very important to me, and the 2-3 weeks following surgery is a critical time in the healing process. Just contact me if you have concerns. I am very particular and specific in my post-op recipe for rhinoplasty, as are most specialist rhinoplasty surgeons.
Rhinoplasty is both an art and a science, and it needs to be me that guides your recovery, not generic health advice, Google, YouTube, another health professional or even another doctor.
How to contact me
During business hours
Contact Raelene, my secretary. She will know where I am and how soon I’m available.
Phone: 03 9347 0680
Email: [email protected]
Email only if non-urgent. Emails after 5pm are not read until the next business day.
For public patients, please contact the Royal Victorian Eye and Ear Hospital (RVEEH) at (03) 9929 8666 and ask to speak to the Rhinology Fellow. They work with me directly and will likely have been involved in your case.
After hours/weekends
Please contact the Epworth on (03) 9483 3833
Do this regardless of which Epworth campus you had your surgery.
State you have had surgery with me, and your post-op instructions specify the Epworth will message Dr Jumeau if needed. They are familiar with this. If you have not heard back within an hour or two, call them again, as I endeavour to get back to everyone as promptly as I can. Don’t call Epworth Hawthorn as it is a Day Surgery and not open outside business hours.
For public patients, contact the Royal Victorian Eye and Ear Hospital and ask to speak to the ENT registrar on call (03) 9929 8666
Emergency
If you are bleeding profusely, have badly damaged your nose or have an emergency unrelated to your nose (Car accident, chest pain, etc.), attend your nearest emergency department or call an ambulance and notify me as soon as you can. I prefer to have you or a family member call me as soon as possible in these circumstances for me to help guide what you do and what gets done at Emergency to not damage your nose. Make sure somebody lets me know. Emergency staff will not always call. Have a phone on you so I can stay in contact as needed.
Dr Philip Jumeau
March, 2024